Toothbrush
For most patients, a power toothbrush is the best choice. Studies show power toothbrushes are much more effective at cleaning teeth by removing plaque and stain effectively, particularly for those who have a history of tooth decay, gum disease, difficulty brushing or who have limited manual dexterity. Dr. Britten often recommends the Sonicare® Platinum toothbrush, as it is shaped like a traditional toothbrush head, and aids in effective plaque removal and gum stimulation and massage.
If not using a power toothbrush, a soft-bristled brush is best for removing plaque and debris from your teeth and along the gum line. Small-headed soft bristled toothbrushes are also preferred, as they can reach areas way in the back of the mouth. Dental professionals generally encourage their patients to pick whatever shape and size is most comfortable. The best toothbrush is one that fits your mouth and allows you to reach all teeth easily.
Replace your toothbrush (or power toothbrush head) when it begins to show wear, or every three months, whichever comes first, or after any illness.
Toothpaste
Unless your dentist recommends otherwise, it’s important to use toothpaste that contains fluoride, which helps to strengthen the outer tooth enamel of our teeth. However, if you are allergic to fluoride, you may want to choose a different toothpaste. Be sure to speak to your dentist or physician before making this switch.
Sometimes a higher, or prescription-level dosage of fluoride is necessary for patients with sensitive teeth, exposed roots, or at greater risk for tooth decay. Dr. Britten often prescribes Clinpro 5000 toothpaste, which contains a therapeutic level of fluoride, in addition to calcium and phosphate, other minerals that help strengthen enamel and the roots of the teeth.
Dr. Britten prefers toothpastes without added harsh chemicals. Some tartar control, whitening, or flavorings burn or irritate the soft tissues of the mouth (inside of lips, cheeks, the tongue, or even the gum tissues). Some toothpastes, especially those with added whitening agents, are abrasive to the enamel and over time can wear it away slowly. Ask your dental professional which products they recommend for whitening or tartar control.
Rinses
Mouthwash and fluoride mouth rinse are two different products. Anti-bacterial mouthwashes (like Listerine) are more effective in controlling plaque than fluoride rinses, and also freshen breath. Fluoride rinses (like ACT brand) coat the teeth with fluoride to strengthen teeth to prevent tooth decay and cavities. They also freshen breath.
Many mouthwashes contain alcohol, so always read the label before giving mouth rinse to a child or someone with a history of substance abuse. Your dental professional may recommend an alcohol-free mouthwash, or to dilute with 1:2 or 2:3 parts’ water.
There are other antimicrobial (Chlorhexidine) or fluoride (Perio-Med) rinses that Dr. Britten recommends available by prescription as needed.
Clean between the teeth at least once per day to remove dental plaque from areas not reached by tooth brushing alone and where tooth decay and gum disease often occur!
Floss
Flossing is critical for healthy gums. Floss is available in many different sizes, coatings, flavors and forms. If you have trouble using the floss around your fingers, you can purchase floss holders in most drugstores and grocery stores. Dr. Britten recommends a floss with texture, rather than a slippery, waxy floss, which will leave a plaque residue behind.
Two of our favorites: Listerine "Gentle Gum Care" , (formerly Reach brand) woven floss. The soft cloth material protects your sensitive gums while effectively removing sticky plaque build up. This soft, springy and resilient dental floss removes plaque effectively and is easier on the gum line.
POH No Wax floss has many thin strands of nylon which enable our floss to disrupt and disorganize sticky bacterial plaque, which is the key to preventing tooth decay and gum disease. It won't just slide over plaque. The multiple strands of tiny nylon slip easily between the closest teeth, able to get just under the gum line.
LISTERINE® ULTRACLEAN® Dental Floss has shred-resistant technology to stretch, flex and glide for an ultimate clean. Its MICRO-GROOVES® technology removes 2x more plaque than Glide® Mint Floss.
How to floss: Place the floss around your index and middle fingers, make a C shape around each tooth and use a push-pull and up and down motion to remove plaque at and below the gum line and between the teeth. Try to be gentle when placing the floss below the gum line.
Children should floss once a day with the assistance of their parents. Many people floss just before bedtime. But if another time is more convenient for you, do it then.
Water Irrigation Devices (such as Sonicare Air Flosser or Waterpik)
Water irrigation devices can remove food from between teeth. Children or teenagers with braces or other orthodontic appliances may find these devices useful to remove food debris and plaque from the teeth and gum line. These devices have shown reductions in bleeding, gingivitis (inflammation of the gums) and plaque accumulation.
Water irrigation devices are most effective when used along with tooth brushing and manual removal of plaque between the teeth with dental floss or other interdental aids and should not ever replace your toothbrush or floss! Also, proper angulation and power settings will avoid injuring thin gum tissues, which may lead to gum recession.
Interdental Brushes or Picks
Dr. Britten recommends using plaque between the teeth using interproximal brushes, go-betweens or soft-picks. These are great tools which remove dental plaque from areas between the teeth most commonly missed by toothbrushing alone. As a popular and effective alternative or addition to dental floss, we recommend GUM® brand Proxabrushes®, Soft-Picks ® or Go-Betweens® are safe and easy to use for cleaning between natural teeth and around crowns, bridges, dental implants and orthodontic appliances.
Proxabrush (Interdental brushes)
Between-teeth cleaning with interdental brushes such as GUM® Proxabrush Go-Betweens® cleaners is as effective as dental floss in removing plaque but is perceived to be much easier and more convenient.
These products are available on long handles (size of a toothbrush handle) or travel-size making it easy to carry the Go-Betweens® cleaners in your pocket or purse for use outside of the home.
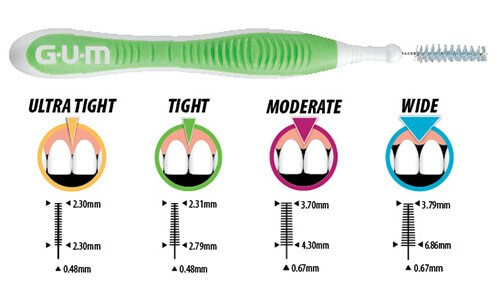
The soft nylon bristles have an antibacterial coating** to help keep the brush clean and hygienic between uses. Different sizes of brush heads are available to fit from the tightest to widest of between teeth spaces. Tight brush heads are designed to clean the tooth and gum surfaces adjacent to the tight spaces.
In four diameters: Ultra Tight, Tight, Moderate and Wide brush heads. Choose the diameter that easily fits into the spaces between the teeth, under the bridge, or around the wires and brackets of an orthodontic appliance.
HOW TO USE
Use gentle in-and-out motions in the spaces between teeth and implants and around crowns and bridges to remove dental plaque and food particles.
- Never force the brush into tight spaces.*** Do not bend or twist wires during use.
- Rinse the brush and handle after each use.
***If a space is too tight to accommodate the smallest Ultra Tight brush, consider using string floss of a Soft-Pick in that space.
GUM® Soft-Picks®: For healthy gums and a great-looking smile, GUM® Soft-Picks® are the convenient way to effectively remove food, plaque and massage gums.
GUM® Soft-Picks®: For healthy gums and a great-looking smile, GUM® Soft-Picks® are the convenient way to effectively remove food, plaque and massage gums.
Dr. Britten and his hygienists are trained to help you select the appropriate oral hygiene aids for your maximum oral health and plaque removal. For more information regarding other oral hygiene aids that Dr. Britten recommends, visit
http://brittenperio.com/oral-health/oral-hygiene/